If you follow my writings, you know I appose Physician-Assisted Suicide. It is not a spiritual or religious issue; we live in a Country where religious decisions are personal and private. I do not have a general objection to the concept of suicide; there may be a time when it seems to be a reasonable alternative. No my vehement opposition is more basic; I object because it contains the word “Physician.”
Mend when possible, and treat suffering always. However, doctors do not kill. To confuse the role of the executioner and the healer is to risk transformative chaos in the physician-patient relationship.
The damage that medically-assisted-suicide can do was pointed out harshly during an especially difficult series of conversations with a family in pain. Such end-of-life, advanced disease, prognosis verses potential discussions are common; I have them every day. Nonetheless, the request, which evolved from this particular conversation, revealed the Kafkaesque nightmare we invite when we involve doctors in actively ending life.
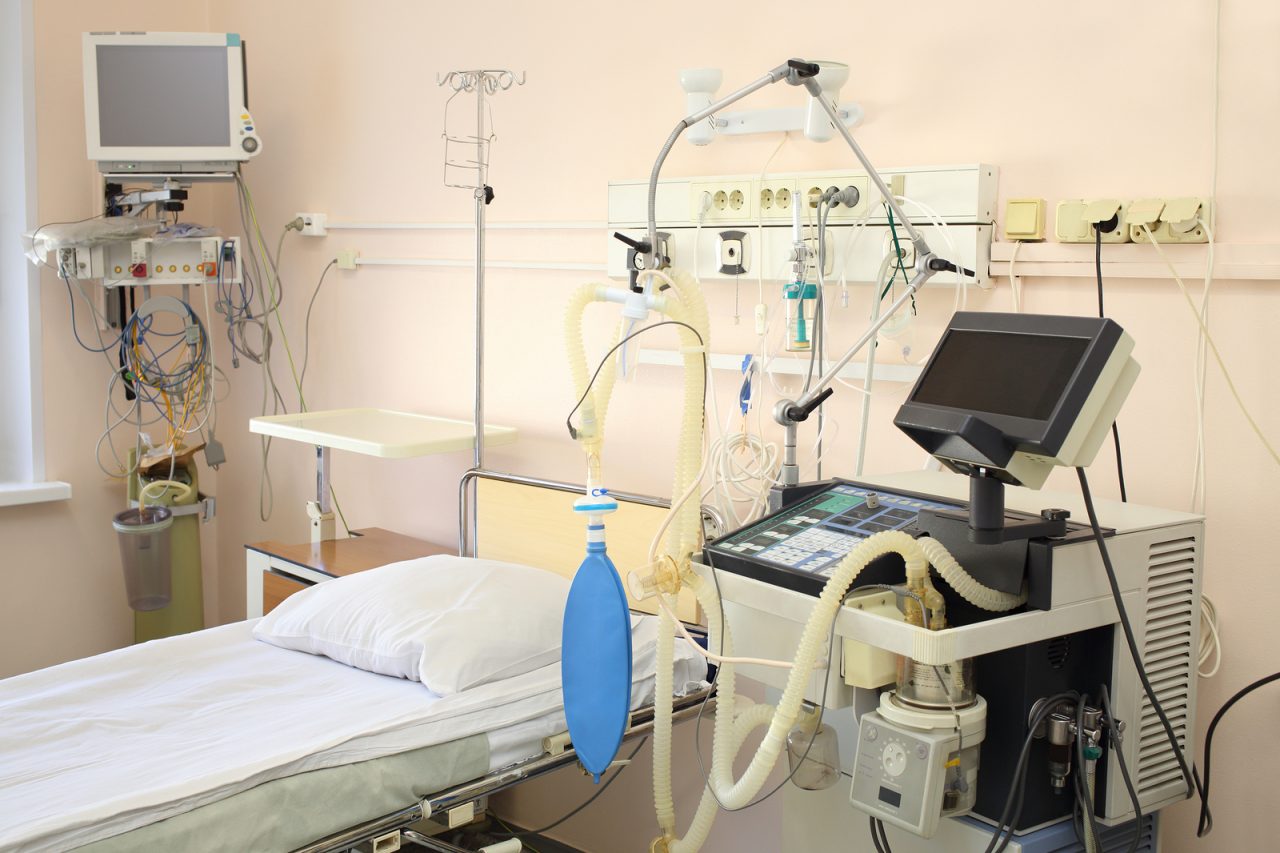
Entering Room 7 of the intensive care unit, the gentle sighs of a respirator and barely audible toll of the cardiac monitor greet me. The patient is on his back, tube passing between lips, chest rising rhythmically with the machine’s breath. Despite brain damage and the IV drips which enter his body thru a spider nest of IV tubing at the base of his neck, he turns briefly toward me during my exam, although his eyes do not focus. Arms wasted and bruised, legs swollen, urine drips into a bag stained red, he appears relaxed, no grimace, no strain, no apparent pain, not short of breath. This is a blessing, because damage from the ravage of disease means that simply to be awake can be agony.
Close are his wife, grasping his right hand and two daughters, who are holding hands together. His elderly mother, in a chair to his left, is squeezed next to the ventilator’s silver cabinet. They respond to my entrance, the wife with a brief, half smile, half grimace. We watch him in silence for a while and then file out, walking down the hall to the conference room.
“How are you doing?” I ask. “Have you gotten any sleep?”
“We’ve been taking shifts,” Answers the younger daughter, face puffy, hair thick.
“Have you all had something to eat?”
“Just coffee, this morning,” Responds his wife, obviously exhausted, blouse wrinkled, mascara stains on each cheek and sleeve.
“It is very important that you eat. When we’re done here, you should all go down to the cafeteria and have some breakfast. You can use the break.”
Nods around, but eyes on the table or the opposite wall, where a cheap framed print of a lighthouse, somewhere, not here, beckons.
“Did you have a chance to discuss what we talked about yesterday?”
“Yes, we talked a lot.”
“What do you think?”
“Well, we had a couple of questions.”
“OK.”
“First, just so we’re clear, you said that this cancer is always incurable. That there is no special center, no expert, no research, where we should take him?”
“There is never anything wrong with getting a second or even a third opinion, but there is no research that has not had success as yet with his cancer. Also, he is too sick for any experiment and too weak to move. Finally, there is no conventional treatment which can cure him.”
“But, you said chemo can sometimes help.”
I hesitate. “I said that when the cancer is this advanced, there is a small chance that chemotherapy might make a small difference.”
“How small?”
“It might shrink the tumors, a little. Maybe it could extend life for a couple of weeks or months.”
“No, I mean how small is the chance that the chemo will help?”
“Probably, not more than 5 or 10%. I also said that he was too sick for chemo.”
“Why?”
“His liver and kidneys are so damaged, his immune system is weak, and his nutrition is depleted, that he would probably not tolerate the chemo.”
“What would happen?”
“He would get mouth sores, diarrhea, fevers, bleeding and probably it would finish off his kidneys. In the end he would die.”
“How likely is that?”
“How likely is it that the chemo would kill him?”
“Yes.”
“Maybe as much as 80%.”
Silence. Outside, in the hall, overhead, I hear my name paged. I ignore it.
“Well, we talked about it and this is what we decided. We want you to give him the chemo.”
“I am not sure I understand.”
“Well, it is worth the chance, so give him the chemo.”
“Let me be clear. The chemo will probably kill him and it will be nasty. The chemo is very unlikely to help him, and the benefit would be very small. If we give him chemo, it would be like planning to kill him, with the tiny chance of a very small shrinkage of cancer. We probably would increase his suffering. He would still have an incurable cancer and he would still die.”
“Look. This is what we think. In some parts of the country, it is legal for a doctor to give medicine to kill a patient. This is better than that. We will give him medicine to probably kill him, but maybe, just maybe, there would be a miracle and he would get better.”
For hundreds of years healers have relied on the ethical idea of “double effect.” That is the concept, especially important with pain medication in dying patients, that if your goal, in your heart-of-hearts, is to treat pain or other suffering, that if there is a side effect which harms the patient, for example a pain medicine slowing breathing, it would ethically acceptable.
What this family was requesting is the antithesis and has no ethical base. I might suggest it is inhumane. Plan to kill, plan to cause suffering, but hope that a miraculous event will occur. This idea stands in direct opposition to the most basic concepts of quality of life and compassion.
This inversion of the goals threatens every patient and every relationship. This establishes a bizarre precedent where we can justify any action, any side effect, because we aim for the worst and simply pray for something good to happen.
In that sort of a world, there is no risk we will not take and no amount of suffering we will not condone. Transplant a new heart into someone with Alzheimer’s. Take off two legs, two arms in a diabetic with pancreatic cancer. Dialysis on a 102 year old with end-stage heart disease. Death and suffering would be confused or equated with healing.
We did not give my patient chemo. After I got over my shock, I spent a long time explaining to the family that what they were requesting is that we not only greatly increase suffering, but that suffering would be our most achievable goal. Eventually we agreed to try and achieve what was most likely and most merciful. Comfort, for whatever time he still has, and perhaps the chance to share a few moments with the ones he loves and who love him.
Many times I have heard the question, “do you believe that physician-assisted suicide” is the start of a slippery slope? Do you think it will lead to killing people who are not terminally ill, but are weak, depressed, poor or simply different? With proper controls, that seems unlikely.
However, perhaps this story warns that we risk another fall, another slope. Perhaps we may lose track of our hopes, goals and the ideals of healing. Slip away from the closeness and mending powers of the physician-patient relationship. We just might find ourselves falling into a darkness that threatens each of us.






19 Comments